The Anatomy of the Procedure: Clinical Factors Shaping Dental Implant Reconstruction
Modern dental implant reconstruction represents a sophisticated intersection of anatomical understanding, material science, and precise surgical planning. The success of these procedures depends on multiple clinical factors that work together to create stable, functional tooth replacements. From initial bone assessment to final crown placement, each step involves careful consideration of individual anatomical variations and structural requirements.
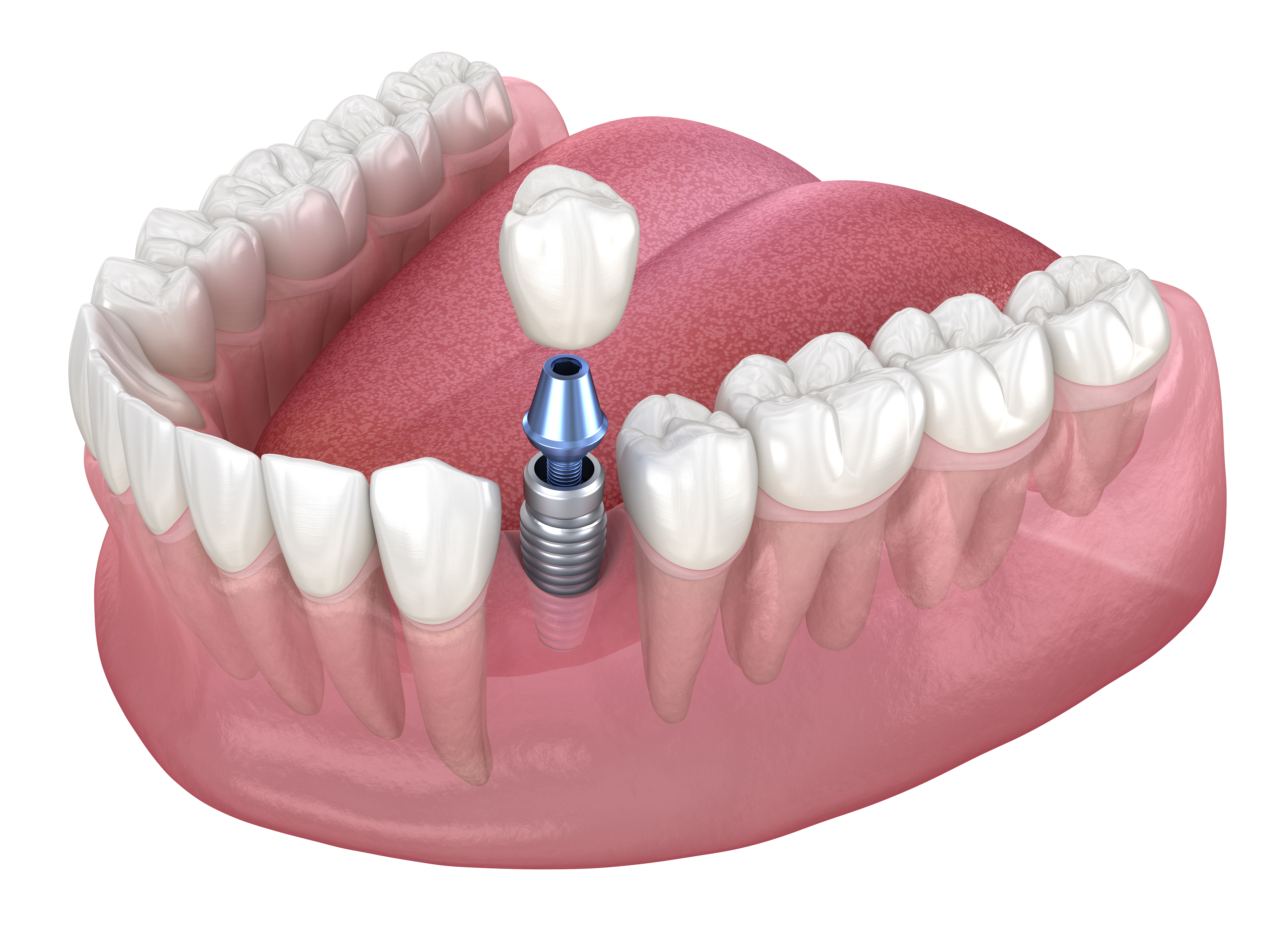
The Transition from Visible Crowns to Foundational Root Structures
Dental implant reconstruction involves replacing both the visible crown and the underlying root system that anchors teeth to the jawbone. The visible portion represents only a small fraction of the complete tooth structure, while the foundation extends deep into the bone tissue. Understanding this transition helps explain why implant procedures require multiple phases and careful attention to structural integration.
The root portion of natural teeth provides stability through direct bone contact and specialized connective tissues. Implant reconstruction recreates this foundation using biocompatible materials that encourage bone integration over time. This process transforms the jawbone architecture to accommodate artificial root structures while maintaining the natural mechanics of chewing and speaking.
How Replacing Missing Teeth Improves Daily Comfort and Speaking Ability
Missing teeth create functional challenges that extend beyond aesthetic concerns. The absence of even a single tooth can alter bite patterns, speech clarity, and jaw alignment. Neighboring teeth may shift position over time, creating additional complications that affect overall oral function.
Implant reconstruction addresses these issues by restoring proper tooth spacing and bite mechanics. The stable foundation allows for normal chewing patterns and clear speech articulation. Unlike removable alternatives, implants provide consistent support that doesn’t shift during eating or speaking activities.
Understanding the Structural Planning Required for Long-Term Stability
Successful implant reconstruction requires comprehensive structural analysis before any surgical intervention begins. This planning phase evaluates bone density, anatomical landmarks, and the relationship between adjacent teeth. Digital imaging provides detailed maps of internal bone structure and identifies potential complications.
The planning process also considers the mechanical forces that will act on the implant during normal function. Chewing generates significant pressure that must be distributed properly through the bone structure. Proper angulation and positioning ensure that these forces enhance rather than compromise long-term stability.
Mapping the Jawbone Layout for Precise Placement
Modern diagnostic techniques create detailed three-dimensional maps of jawbone architecture. These maps reveal bone thickness, density variations, and the location of vital structures like nerves and blood vessels. Accurate mapping enables precise implant placement that maximizes stability while avoiding anatomical complications.
The mapping process identifies optimal placement angles and depths for each individual case. This information guides the creation of surgical templates that ensure consistent positioning during the actual procedure. Digital planning reduces surgical time and improves predictability of outcomes.
Evaluating the Initial Foundation for Everyday Chewing Strength
The strength of the initial bone foundation determines the timeline and approach for implant reconstruction. Dense bone provides immediate stability and may allow for faster loading protocols. Areas with softer bone require longer integration periods before normal chewing forces can be applied.
Foundation evaluation includes assessment of both quantity and quality of available bone tissue. Some individuals may require bone grafting procedures to create adequate foundation support. These preparatory steps ensure that the final restoration can withstand the mechanical demands of daily function.
The Mechanics of Preparing the Jawbone for a Strong Structural Foundation
Bone preparation involves creating a precisely sized cavity that matches the implant dimensions. The preparation process generates controlled trauma that stimulates the natural healing response. This response encourages new bone formation around the implant surface, creating the integration necessary for long-term stability.
The mechanical aspects of bone preparation require careful attention to temperature control and irrigation. Excessive heat during drilling can damage bone cells and compromise integration. Proper technique preserves the biological environment while creating the exact geometry needed for optimal implant stability.
| Clinical Stage | Procedural Function | Complexity Tier |
|---|---|---|
| Initial Assessment and Digital Mapping | Comprehensive bone evaluation and surgical planning | Standard titanium materials with basic crown fabrication |
| Bone Preparation and Implant Placement | Precise cavity creation and implant insertion | Enhanced zirconia components with custom laboratory work |
| Integration and Healing Monitoring | Biological bonding assessment and tissue management | Premium materials with advanced surface treatments |
| Final Restoration and Functional Testing | Crown attachment and bite adjustment | Complete aesthetic reconstruction with specialized components |
How Individual Bone Density Influences the Overall Timeline of the Process
Bone density varies significantly between individuals and even within different areas of the same mouth. Dense bone provides immediate stability but may require longer periods for complete integration. Softer bone integrates more quickly but needs extended healing time before full function can be restored.
The timeline for implant reconstruction adjusts based on these density variations. Some cases may proceed to final restoration within a few months, while others require extended healing periods. Individual factors such as age, health status, and bone metabolism all influence the integration timeline.
Understanding Why Some Individuals Require Additional Preparatory Steps
Anatomical variations and previous dental history can necessitate preparatory procedures before implant placement. Insufficient bone volume may require grafting to create adequate foundation support. Gum tissue irregularities might need correction to ensure proper healing and aesthetic outcomes.
These preparatory steps are determined during the initial assessment phase. While they extend the overall timeline, they significantly improve the likelihood of long-term success. Each additional procedure addresses specific anatomical challenges that could otherwise compromise the final result.
The Natural Bonding Phases Required Before Enjoying Normal Meals
Bone integration occurs in predictable phases that must be respected for optimal outcomes. The initial healing phase involves blood clot formation and early bone cell activity. The intermediate phase sees new bone formation around the implant surface. The final phase achieves mature bone integration that can support full chewing forces.
Each phase has specific dietary recommendations that protect the developing integration. Early phases may require soft food diets, while later phases gradually allow return to normal eating patterns. Understanding these phases helps set realistic expectations for the recovery timeline.
Recognizing the Importance of a Solid Base for a Confident Smile
The foundation created during implant reconstruction directly impacts both function and aesthetics. A stable base allows for natural-looking crown contours and proper gum tissue architecture. This stability also provides the confidence that comes with knowing the restoration will perform reliably during daily activities.
The psychological impact of a solid foundation extends beyond mere function. Knowing that the replacement tooth is securely anchored allows for natural speaking and eating patterns. This confidence contributes to improved quality of life and social interactions.
Dental implant reconstruction represents a sophisticated approach to tooth replacement that addresses both immediate functional needs and long-term stability requirements. The success of these procedures depends on careful attention to anatomical factors, proper material selection, and respect for biological healing processes. Understanding these clinical factors helps individuals make informed decisions about their oral health restoration options.




