What Modern Dental Implants Actually Are and Which Structural Factors Shape the Finished Restoration
A modern dental implant represents a complete mechanical system where a manufactured titanium post becomes permanently embedded in jaw bone tissue and supports a visible ceramic or porcelain restoration above the gum line. This fixed assembly replaces missing tooth structures through direct physical integration rather than adhesive attachment or removable hardware. The finished installation depends on precise dimensional relationships between the buried anchor, the connecting abutment component, and the final crown or bridge that handles daily chewing forces.
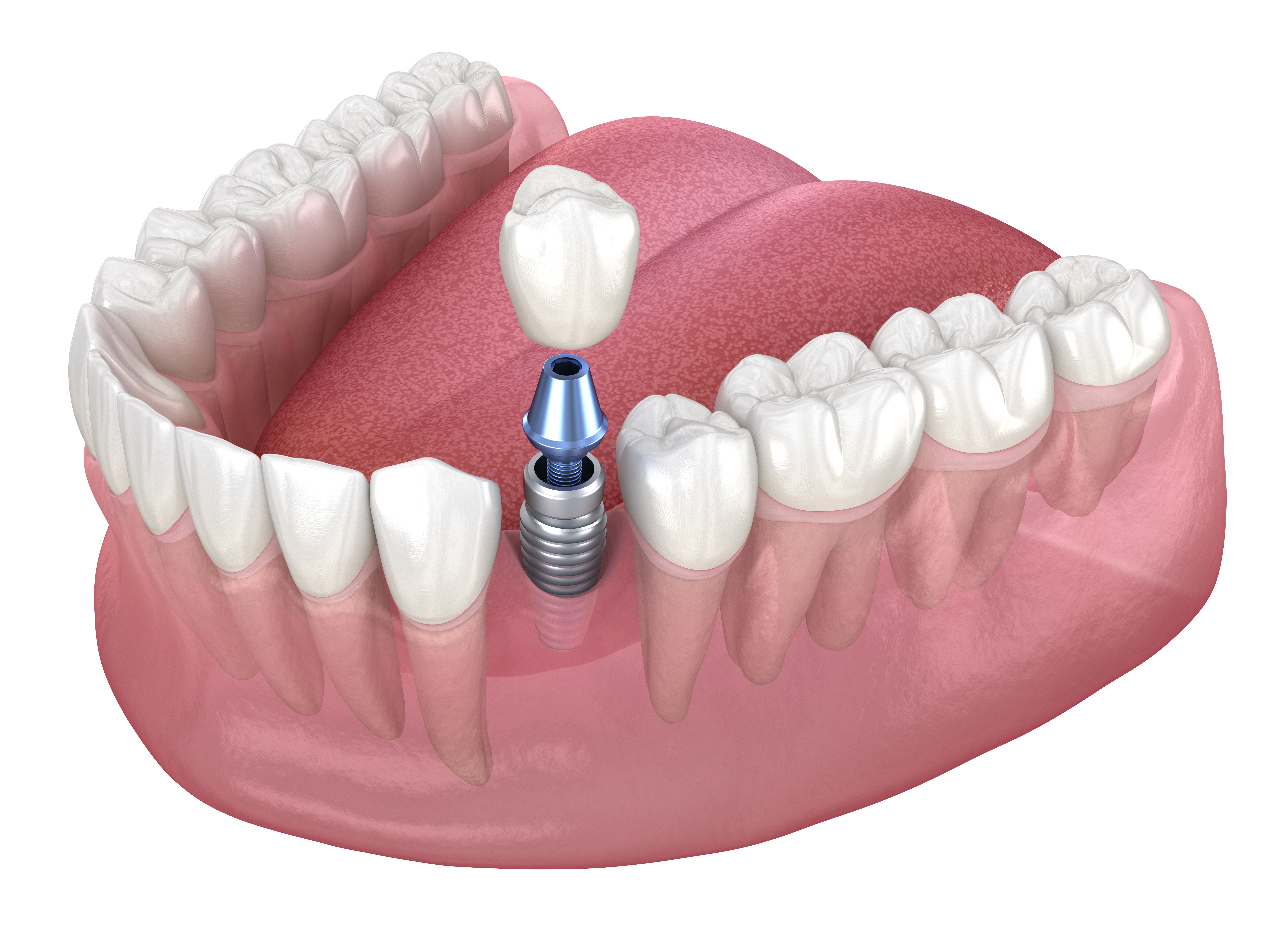
The fundamental architecture of a contemporary dental implant consists of three distinct physical layers working as a unified load bearing structure. At the foundation sits a threaded titanium cylinder that penetrates through soft gum tissue and embeds directly into the mineralized jaw bone below. This buried anchor measures between eight and sixteen millimeters in length depending on available bone depth, with surface textures and thread patterns engineered to maximize immediate contact area with surrounding bone tissue. The metal composition typically uses commercially pure titanium or titanium alloy grades that demonstrate biological compatibility and resist corrosion when exposed to saliva and tissue fluids over decades of continuous use.
How an Advanced Dental Implant Functions as a Permanent Structural Anchor Secured Directly Into the Jawbone Without Affecting Neighboring Teeth
The threaded titanium post creates mechanical stability through a process where living bone cells gradually colonize the textured metal surface and form direct molecular bonds with the implant exterior. Specific titanium thread designs create immediate mechanical stability and allow continuous physical integration with surrounding tissue as new bone matrix deposits onto the implant threads over a period spanning several months. This biological welding process differs fundamentally from natural tooth attachment, where fibrous ligaments suspend the root within a socket and permit microscopic movement. The rigid implant connection transfers chewing forces directly into the supporting jaw structure without involving adjacent teeth, eliminating the need to reshape healthy enamel on neighboring teeth that traditional bridge frameworks require.
The precision milled abutment connection provides a sealed transition zone between the hidden base and the visible restoration through either an internal hex socket or morse taper interface machined into the implant top. This connecting junction must resist rotational forces, prevent bacterial penetration into the threaded cavity, and maintain dimensional accuracy measured in micrometers to avoid gaps where tissue inflammation could develop. Advanced material composition ensures the entire supporting foundation resists continuous daily chewing forces without metal fatigue, as human bite forces can exceed 200 pounds per square inch during grinding motions on posterior teeth. The finished physical geometry maintains natural jawline contours and supports balanced vertical load distribution across the mouth by positioning the implant crown at the correct height and angle relative to opposing teeth.
How the Physical Integration of Advanced Implants Often Requires Preparatory Bone Grafting to Establish Sufficient Structural Depth
Successful long term implant stability depends on adequate bone volume surrounding the titanium threads on all sides, typically requiring at least two millimeters of healthy bone tissue encasing the implant circumference. High resolution digital planning models map the exact foundational bone volume before any physical placement begins, using cone beam computed tomography scans that reveal bone density values and anatomical structures like nerve canals or sinus cavities that must be avoided during drilling. When natural bone height or width falls below minimum thresholds, supplemental grafting procedures deposit processed bone mineral particles into deficient areas months before implant insertion, allowing time for the graft material to consolidate into load bearing tissue.
Customized physical templates guide the specific positioning depth to maximize contact with the strongest available foundational bone, ensuring the implant axis aligns with the planned crown emergence angle and avoids tilting that could create uneven stress concentration. Adjusting the spatial distance between multiple titanium posts ensures adequate blood supply and continuous structural stability when replacing several adjacent teeth, as implants placed too close together can compromise the bone bridge between fixtures and lead to eventual bone loss. Specific baseline foundation requirements determine the ultimate physical complexity of securing the permanent base, with cases involving severe bone atrophy potentially requiring months of staged grafting before implant placement becomes mechanically viable.
How Heavy Continuous Zirconia Bridges Require Multiple Distributed Anchor Points to Manage Significant Physical Weight Across the Span
Replacing multiple consecutive teeth demands careful calculation of how many implant anchors will support the prosthetic span without overloading individual posts. Creating an individual ceramic crown demands precise architectural contact clearances with adjacent teeth for straightforward daily cleaning, maintaining gap dimensions that permit floss passage while preventing food impaction in the interdental space. Screw retained prosthetic designs leave hidden access channels and allow straightforward physical removal for future maintenance, with small composite plugs concealing the screw holes on the chewing surface after the crown has been tightened onto the abutment.
Aligning the final chewing surface physically redistributes mechanical pressure and protects the outer porcelain from structural chipping by ensuring even contact during jaw closure and lateral grinding movements. A tight soft tissue seal around the titanium neck creates a physical barrier and prevents debris accumulation beneath the restoration, requiring the gum margin to adapt snugly against the polished abutment collar in a manner similar to how healthy gum tissue surrounds natural tooth enamel. The prosthetic design must account for both vertical biting forces and horizontal shearing stresses that occur during chewing, with implant supported bridges typically featuring reinforced frameworks of zirconia or metal substructures beneath the aesthetic porcelain veneer.
How the Completed Advanced Implant System Replaces Removable Plastic Components With a Fixed Mechanical Structure Anchored Permanently Within the Underlying Jaw
The transition from removable dentures to fixed implant restorations eliminates the acrylic palate covering that blocks taste sensation and the metal clasps that place stress on remaining natural teeth. The physical alignment of the final ceramic surface controls the specific air flow required for clear speech articulation, particularly for front teeth that shape sounds like F, V, S, and TH through precise tongue and lip positioning against the tooth edges. Transferring vertical chewing pressure directly to the foundational bone provides continuous mechanical support for the surrounding facial geometry over time, as the stimulation from biting forces helps maintain bone density that would otherwise gradually resorb following tooth loss.
The manufactured transition between the implant collar and the natural gum line requires precise physical shaping to eliminate food trap voids where bacteria could colonize and trigger inflammation in the surrounding soft tissue. Continuous daily use relies on the immovable physical connection between the titanium post and the heavy upper restoration, creating a unified structure that functions as a single rigid unit rather than the slight mobility present in natural tooth suspension. The ceramic crown material itself must withstand thermal cycling from hot and cold foods, resist staining from dietary pigments, and maintain surface gloss despite abrasive contact with toothbrush bristles and opposing enamel during thousands of daily chewing cycles.
How the Structural Scope of Different Dental Implant Systems Emerges Clearly During Side by Side Digital Comparison
Manufacturers produce implant systems with varying thread geometries, surface treatments, and connection designs that influence initial stability and long term integration outcomes. Stated online prosthetic features match visible physical realities like titanium thread geometry, with aggressive thread pitches providing greater initial grip in soft bone while finer threads suit dense bone types. Digital search tools help spot deviations in foundational integration details before an actual clinical consultation begins, allowing comparison of published research data on integration rates, mechanical complication frequencies, and documented long term survival statistics across different implant brands and designs.
| Structural Component | Physical Reality | Daily Use Consequence |
|---|---|---|
| Threaded titanium post body | Commercially pure grade four titanium and rough acid etched surface texture and lengths from eight to sixteen millimeters | Direct bone contact without intervening ligament and permanent rigid fixation and zero mobility during function |
| Internal hex abutment connection | Precision machined hexagonal socket and anti rotational geometry and micron level manufacturing tolerances | Prevents prosthetic loosening and creates bacterial seal and allows prosthetic removal for maintenance |
| Custom milled zirconia abutment | Monolithic ceramic material and tooth colored appearance and shaped emergence profile | Eliminates visible metal margins and supports natural gum contours and resists corrosion |
| Screw retained porcelain crown | Layered ceramic veneer and internal metal or zirconia framework and occlusal screw access channel | Permits crown removal without damage and distributes chewing forces and allows future adjustments |
| Cement retained crown design | Permanent adhesive bond and no visible access holes and relies on friction retention | Creates seamless surface appearance and requires crown destruction for removal and simplifies occlusal shaping |
Physical Dimensions and Material Properties That Govern Implant Performance
The diameter of the titanium post influences the surface area available for bone contact, with standard implants measuring approximately four millimeters across while narrow diameter versions accommodate restricted spaces between tooth roots. Platform switching design principles intentionally use a narrower abutment diameter than the implant body diameter, creating a horizontal offset that positions the prosthetic margin inward from the implant edge and helps preserve surrounding bone height. The length of the threaded portion determines how deeply the implant engages the jaw bone, with longer fixtures generally providing greater stability but requiring adequate vertical bone height and clearance from anatomical structures like nerve canals in the lower jaw or sinus cavities in the upper jaw.
Surface roughness at the microscopic level affects how quickly bone cells colonize the titanium exterior, with treatments like sandblasting, acid etching, or calcium phosphate coating accelerating the integration timeline compared to smooth machined surfaces. The taper angle of the implant body influences how drilling forces distribute during placement and how the fixture resists lateral bending moments during function. Modern implant designs incorporate these variables into engineered systems where each dimensional parameter serves a specific mechanical or biological function rather than arbitrary aesthetic choices.
The completed implant restoration represents a permanent addition to the oral architecture that requires the same daily hygiene maintenance as natural teeth, including mechanical plaque removal through brushing and interdental cleaning to prevent inflammatory conditions in the surrounding gum tissue. The structural integrity of the titanium anchor itself rarely fails, with documented survival rates exceeding 95 percent over ten year periods in healthy bone, though the prosthetic components above the gum line may require occasional adjustment or replacement as ceramic materials gradually wear or abutment screws loosen from repeated stress cycles. Understanding the physical composition and mechanical principles underlying each component helps clarify how these engineered systems achieve long term functional stability in the demanding environment of the human mouth.




