What Advanced Dental Implants Actually Are and Which Structural Factors Shape the Finished Restoration
Advanced dental implants represent permanent mechanical structures designed to replace missing teeth through direct integration with jawbone tissue. Unlike removable alternatives, these systems rely on precise engineering principles where titanium posts anchor into bone, abutment connections create sealed transitions, and ceramic restorations distribute chewing forces. Understanding the physical components and their interaction reveals how material choices, dimensional specifications, and assembly geometry determine long-term structural performance in the oral environment.
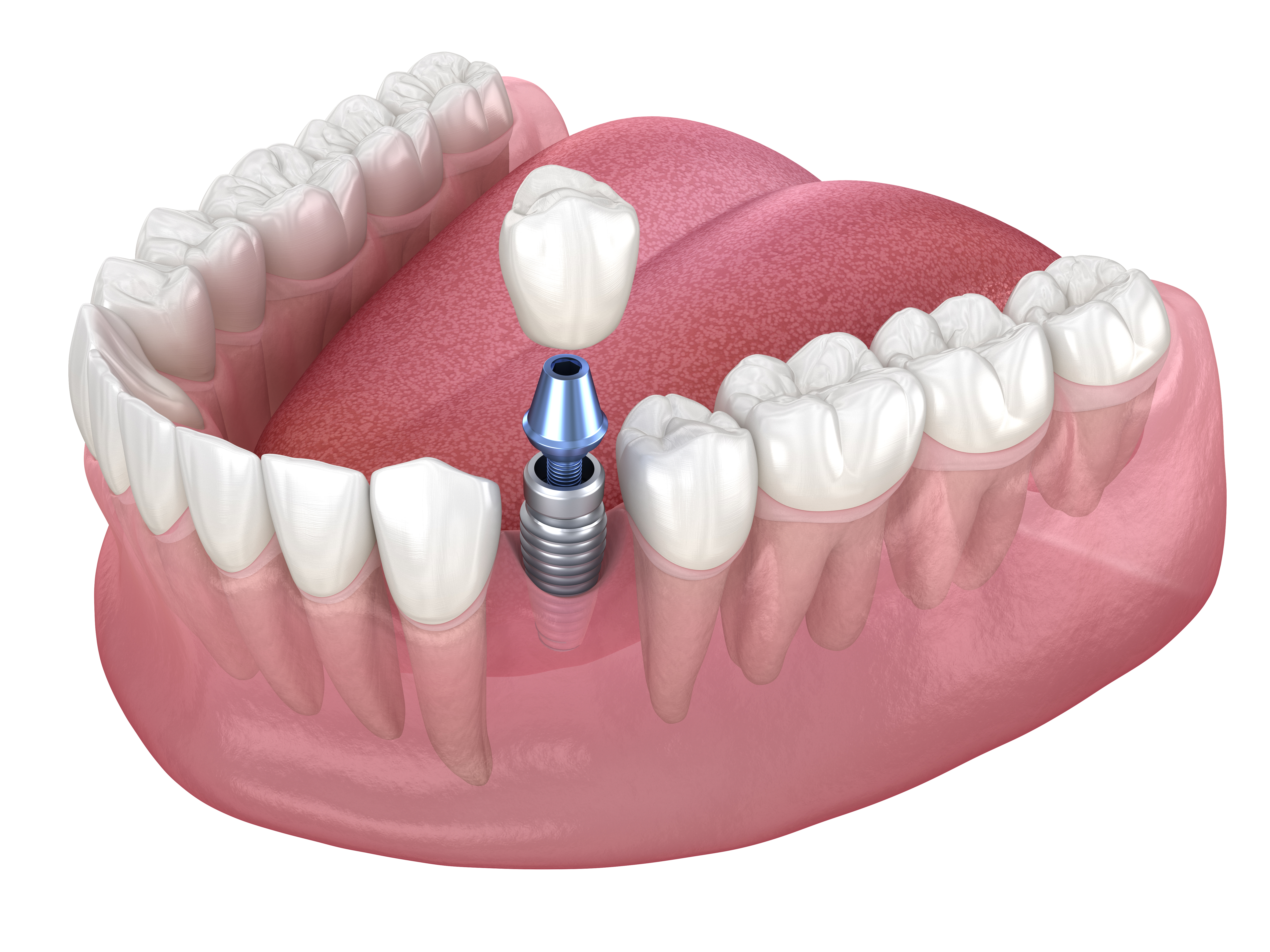
Modern dental implants function as engineered replacement systems where manufactured components work together to restore missing teeth through direct bone integration. The complete assembly involves multiple precision parts that must withstand continuous mechanical stress while maintaining biological compatibility with surrounding tissue.
How Titanium Posts Anchor Into Jawbone Without Affecting Adjacent Teeth
An advanced dental implant functions as a permanent structural anchor secured directly into the jawbone without affecting neighboring teeth. The titanium post penetrates through gum tissue and embeds into the underlying bone structure, creating an independent foundation that stands alone. Specific titanium thread designs create immediate mechanical stability and allow continuous physical integration with surrounding tissue through a biological process where bone cells grow directly onto the metal surface. The precision milled abutment connection provides a sealed transition zone between the hidden base and the visible restoration, preventing bacterial infiltration at the junction point. Advanced material composition ensures the entire supporting foundation resists continuous daily chewing forces without metal fatigue, as grade 4 or grade 5 titanium alloys demonstrate exceptional strength-to-weight ratios. The finished physical geometry maintains natural jawline contours and supports balanced vertical load distribution across the mouth by transferring pressure directly through the artificial root into dense cortical bone layers.
Preparatory Bone Structure and Digital Planning Requirements
The physical integration of advanced implants often requires preparatory bone grafting to establish sufficient structural depth when existing bone volume falls below minimum dimensional thresholds. High resolution digital planning models map the exact foundational bone volume before any physical placement begins, using cone beam computed tomography scans that reveal three-dimensional bone density and anatomical landmarks. Customized physical templates guide the specific positioning depth to maximize contact with the strongest available foundational bone, ensuring the implant threads engage cortical bone rather than softer trabecular tissue. Adjusting the spatial distance between multiple titanium posts ensures adequate blood supply and continuous structural stability, as posts placed too close together can compromise vascularization and osseointegration. Specific baseline foundation requirements determine the ultimate physical complexity of securing the permanent base, with narrow ridges or thin sinus floors necessitating augmentation procedures before implant insertion becomes mechanically viable.
Prosthetic Design Variations and Mechanical Load Distribution
Heavy continuous zirconia bridges require multiple distributed anchor points to manage significant physical weight across the span, preventing cantilever stress that could overload individual implant posts. Creating an individual ceramic crown demands precise architectural contact clearances with adjacent teeth for straightforward daily cleaning, with interdental spaces maintained at 0.5 to 1.0 millimeters to allow floss passage. Screw retained prosthetic designs leave hidden access channels and allow straightforward physical removal for future maintenance, as the restoration attaches through an internal screw rather than permanent cement. Aligning the final chewing surface physically redistributes mechanical pressure and protects the outer porcelain from structural chipping by establishing balanced occlusal contacts that prevent edge loading. A tight soft tissue seal around the titanium neck creates a physical barrier and prevents debris accumulation beneath the restoration, with proper emergence profile shaping encouraging gum tissue to form a protective collar around the implant platform.
Fixed Mechanical Structure and Facial Geometry Support
The completed advanced implant system replaces removable plastic components with a fixed mechanical structure anchored permanently within the underlying jaw, eliminating the movement and instability associated with dentures. The physical alignment of the final ceramic surface controls the specific air flow required for clear speech articulation, as tooth position directly affects phonetic sounds produced during conversation. Transferring vertical chewing pressure directly to the foundational bone provides continuous mechanical support for the surrounding facial geometry over time, stimulating bone remodeling that maintains ridge volume and prevents the facial collapse seen with missing teeth. The manufactured transition between the implant collar and the natural gum line requires precise physical shaping to eliminate food trap voids where bacteria could accumulate and cause peri-implant inflammation. Continuous daily use relies on the immovable physical connection between the titanium post and the heavy upper restoration, with the osseointegrated interface capable of withstanding hundreds of pounds of bite force without loosening.
Structural Component Analysis and Physical Reality
The structural scope of different dental implant systems emerges clearly during side by side digital comparison of manufacturer specifications and published technical data. Stated online prosthetic features match visible physical realities like titanium thread geometry, with variations in thread pitch, depth, and profile affecting primary stability and surface area for bone contact. Digital search tools help spot deviations in foundational integration details before an actual clinical consultation begins, allowing comparison of implant diameters, lengths, connection types, and surface treatments across different product lines.
| Structural Component | Physical Reality | Daily Use Consequence |
|---|---|---|
| Titanium post body | Grade 4 commercially pure titanium and grade 5 Ti6Al4V alloy and threaded cylindrical geometry | Withstands 200 to 500 pounds of bite force and resists corrosion in oral fluids and maintains position for decades |
| Abutment connection | Internal hex and internal conical taper and external hex designs | Prevents rotational movement and creates bacterial seal and distributes stress into implant body |
| Zirconia crown | Monolithic solid zirconia and layered porcelain over zirconia framework | Matches adjacent tooth color and resists staining and handles chewing pressure without fracture |
| Thread design | V shaped and buttress and square thread profiles and variable pitch patterns | Creates immediate mechanical lock and increases surface area and compresses bone during insertion |
| Surface treatment | Sandblasted and acid etched and anodized and hydroxyapatite coated surfaces | Accelerates bone cell attachment and increases osseointegration speed and enhances long term stability |
Material Engineering and Load Bearing Capacity
The interaction between implant components determines overall system performance under real world conditions. Titanium demonstrates biocompatibility through a passive oxide layer that forms instantly upon exposure to air or tissue fluids, preventing immune rejection. The modulus of elasticity for titanium approximates bone more closely than stiffer materials, reducing stress shielding effects that can cause bone resorption around the implant. Zirconia restorations provide aesthetic advantages through translucency that mimics natural enamel while maintaining flexural strength exceeding 900 megapascals. The abutment screw represents a potential weak point where loosening can occur if torque specifications are not maintained, requiring periodic verification of tightness. Cement retained crowns eliminate screw access holes in the visible chewing surface but create challenges for future removal if complications arise.
The dimensional precision of implant manufacturing directly affects clinical outcomes, with tolerances measured in micrometers ensuring proper fit between components. Platform switching designs position the abutment margin inward from the implant edge, concentrating stress away from the marginal bone and preserving ridge height. Tapered implant bodies mimic natural root anatomy and allow placement in extraction sockets, while parallel walled designs maximize thread engagement in dense bone. The implant-abutment junction experiences micromotion during function, and design features that minimize this movement reduce bacterial colonization and inflammatory responses.
Advanced dental implant systems represent complex engineered solutions where material science, mechanical design, and biological principles converge to create functional tooth replacements. The physical characteristics of each component determine how forces transfer through the restoration into supporting bone, affecting both immediate stability and long-term structural integrity. Understanding these mechanical relationships clarifies how different design choices influence the performance and durability of the finished restoration under continuous oral function.




