The Mechanics of Screwless Dental Implants: Structural Innovations in Rehabilitation
Screwless dental implants represent a significant evolution in restorative dentistry, moving away from conventional threaded designs toward friction-fit and press-fit mechanisms. These systems rely on precise biomechanical principles and bioactive surface technologies to achieve stability without traditional mechanical fasteners. Understanding the structural innovations, procedural adaptations, and biological integration processes associated with threadless implant designs provides valuable insight into contemporary rehabilitation approaches.
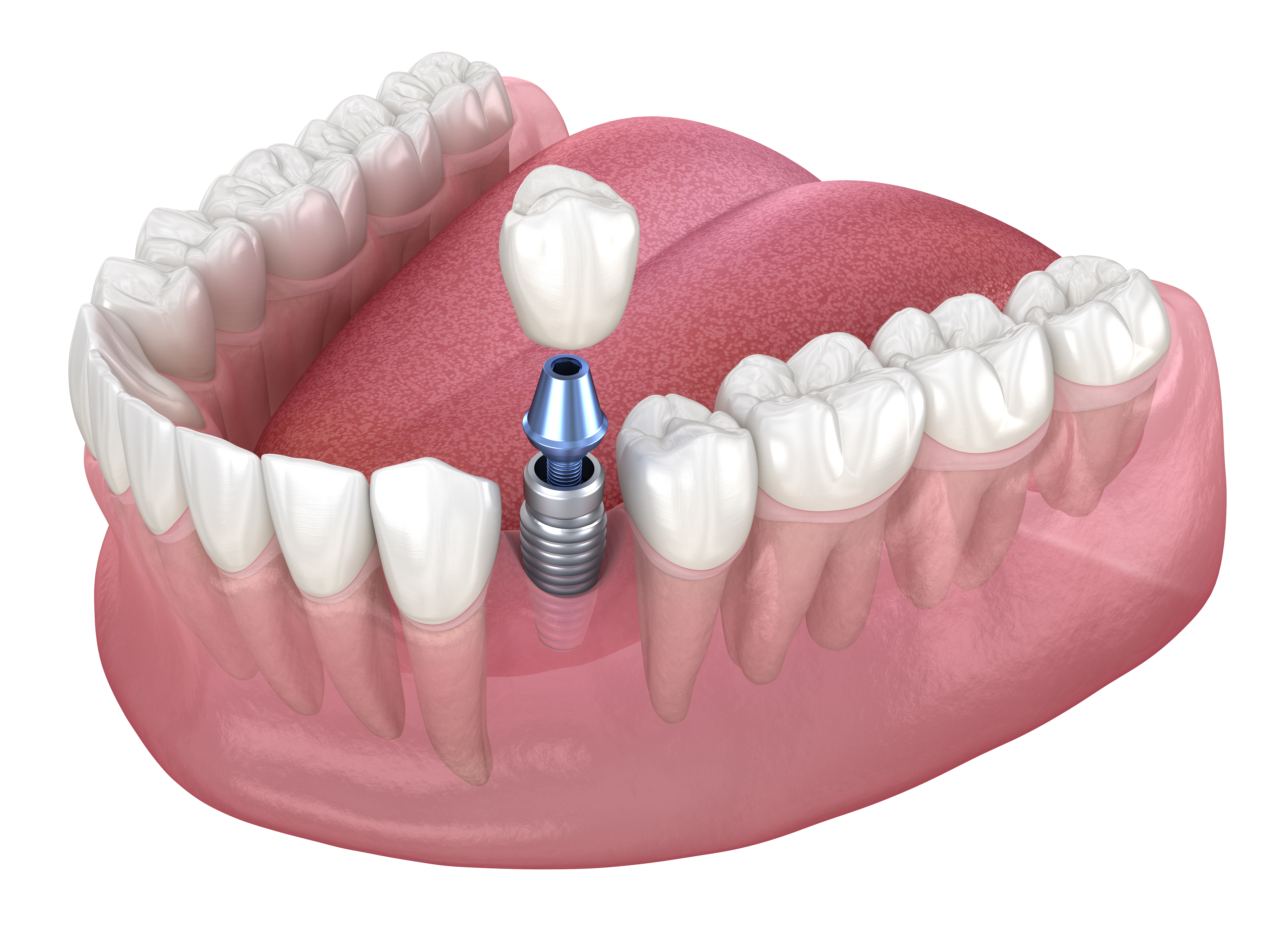
The shift from traditional threaded systems to screwless dental implants marks a notable change in how prosthetic components achieve stability within the jawbone. Conventional implants use helical threads that engage bone through rotational insertion, creating mechanical interlock. Screwless alternatives employ friction-fit mechanisms where the implant body is pressed into a precisely prepared osteotomy site. The absence of threads changes the contact dynamics between the implant surface and surrounding bone, relying instead on compressive forces and surface characteristics to maintain position during the healing phase.
Press-fit technology differs structurally from threaded designs in several ways. The implant body typically features a smooth or minimally textured cylindrical or tapered form that matches the prepared site dimensions with high precision. Insertion occurs through controlled axial pressure rather than rotational force, which can alter the stress patterns introduced to the bone during placement. The elimination of thread grooves creates a continuous contact surface, potentially influencing how loads transfer from the prosthetic structure to the supporting bone during function.
How Friction-Fit Mechanisms Secure Prosthetics Without Mechanical Bolts
Friction-fit implants achieve initial stability through interference fit principles, where the implant diameter slightly exceeds the prepared site, creating compressive contact along the interface. This mechanical grip holds the implant in position immediately after placement, allowing biological processes to begin. Bioactive surface coatings, often incorporating calcium phosphate compounds or micro-textured patterns, encourage cellular activity and bone apposition. These surfaces facilitate the transition from mechanical retention to biological integration, where new bone forms directly against the implant material, creating a structural bond that replaces the initial frictional hold.
The integration timeline for friction-based systems follows a similar biological sequence to threaded implants, though the interface characteristics differ. Osteoblasts migrate to the implant surface, depositing new bone matrix that mineralizes over weeks to months. The smooth or minimally featured surface geometry of screwless designs may influence the rate and pattern of bone contact, though clinical outcomes depend on multiple factors including bone density, surgical technique, and patient physiology.
Procedural Mechanics of Site Preparation for Threadless Insertion
Preparing the surgical site for a screwless implant involves creating a precisely dimensioned osteotomy that matches the implant geometry. Sequential drilling with calibrated instruments enlarges the site to a final diameter that allows the implant to be seated with controlled force. Unlike threaded systems where the final preparation is slightly undersized to allow thread engagement, press-fit protocols aim for an exact dimensional relationship that generates the intended interference fit.
The insertion process applies axial pressure through specialized instruments, avoiding the rotational forces associated with threaded placement. This approach can preserve bone structure by minimizing the shear stresses introduced during implant seating. The elimination of rotational drilling in the final stages may reduce heat generation and mechanical disruption to the surrounding bone matrix, though careful technique remains necessary to prevent excessive force that could cause microfractures.
Soft Tissue Response and Elimination of Micro-Gaps
Smooth implant collars in screwless designs present a continuous surface to the surrounding soft tissue, potentially influencing the mucosal seal that forms around the prosthetic emergence profile. Traditional screw-retained restorations create junctions between components that can harbor bacterial colonization if not properly sealed. Threadless systems often integrate the abutment and implant body into a single structure or use friction-fit abutment connections, reducing the number of interfaces where micro-gaps might form.
Advanced surface texturing at the coronal portion of screwless implants can facilitate soft tissue attachment, creating a biological barrier that helps protect the underlying bone from bacterial infiltration. The absence of screw access channels through the restoration eliminates one potential pathway for fluid and bacterial penetration, which may contribute to the long-term stability of the peri-implant tissues.
Aesthetic Outcomes and Structural Advantages in Visible Zones
In the anterior region where aesthetics are particularly important, screwless implants offer structural advantages by eliminating the screw access hole that typically penetrates the facial surface of screw-retained crowns. This allows the restoration to be fabricated with uninterrupted contours and translucency patterns that more closely mimic natural tooth structure. The solid core construction of friction-fit restorations can enhance the mechanical strength of the prosthetic crown, particularly in thin or highly translucent ceramic materials.
Load distribution in threadless designs differs from threaded systems due to the continuous contact surface along the implant-bone interface. Masticatory forces transfer through the smooth or minimally textured body without the stress concentration points that can occur at thread crests. The solid connection between abutment and implant body in many screwless systems creates a rigid structure that transmits forces efficiently, though the specific biomechanical behavior depends on the implant geometry and material properties.
Clinical Protocols and Procedural Variations
Clinical protocols for screwless implants adapt to the specific anatomical conditions encountered in each case. Bone density plays a significant role in determining the insertion torque and initial stability achieved with press-fit systems. In denser bone types, the interference fit generates higher retention forces, while softer bone may require modifications to the preparation protocol or implant design to achieve adequate primary stability.
Evaluation metrics for press-fit stability include insertion torque values, resonance frequency analysis, and clinical mobility testing. These assessments help determine when the implant has achieved sufficient integration to support loading. Procedural variations exist among different proprietary locking technologies, with manufacturers offering specific instrumentation and protocols tailored to their implant designs.
| Technology Type | Structural Feature | Valuation Indicator |
|---|---|---|
| Cylindrical Press-Fit | Smooth body with interference fit and bioactive coating | Mid-range procedural complexity |
| Tapered Friction-Lock | Gradual taper with micro-textured surface and compression fit | Standard implementation tier |
| Integrated Abutment | Single-piece design with smooth collar and solid core | Specialized application category |
| Ceramic Threadless | Zirconia construction with surface modification and press insertion | Premium material classification |
Procedural variations in screwless implant placement reflect differences in proprietary technologies and clinical requirements. Some systems incorporate specialized surface treatments that accelerate bone integration, while others focus on mechanical design features that enhance initial stability. The choice among available options depends on anatomical factors, aesthetic requirements, and the specific clinical scenario.
Structural Performance in Varied Clinical Scenarios
Press-fit systems demonstrate particular advantages in situations where the elimination of screw-related complications offers clinical value. The absence of screw loosening removes one potential maintenance issue, though the friction-fit connection must maintain integrity under functional loads. In cases where bone quality or anatomical constraints limit the available implant dimensions, the continuous load distribution of threadless designs may provide favorable stress patterns compared to threaded alternatives.
The long-term performance of screwless implants depends on achieving and maintaining biological integration along the implant-bone interface. Clinical studies continue to evaluate survival rates, complication profiles, and patient-reported outcomes across different implant designs and clinical applications. Understanding the structural mechanics and biological principles underlying these systems helps inform appropriate case selection and procedural planning in contemporary restorative practice.




