The Anatomy of Dental Implant Costs: Clinical Factors Shaping the Restoration Process
Modern dental implant procedures represent a sophisticated integration of surgical precision, advanced diagnostics, and material science. The restoration process involves multiple clinical stages where anatomical factors, technological capabilities, and procedural complexity directly influence the overall framework. Understanding these interconnected elements provides insight into how structural mechanics, diagnostic protocols, and material selection create the foundation for successful osseointegration and long-term stability.
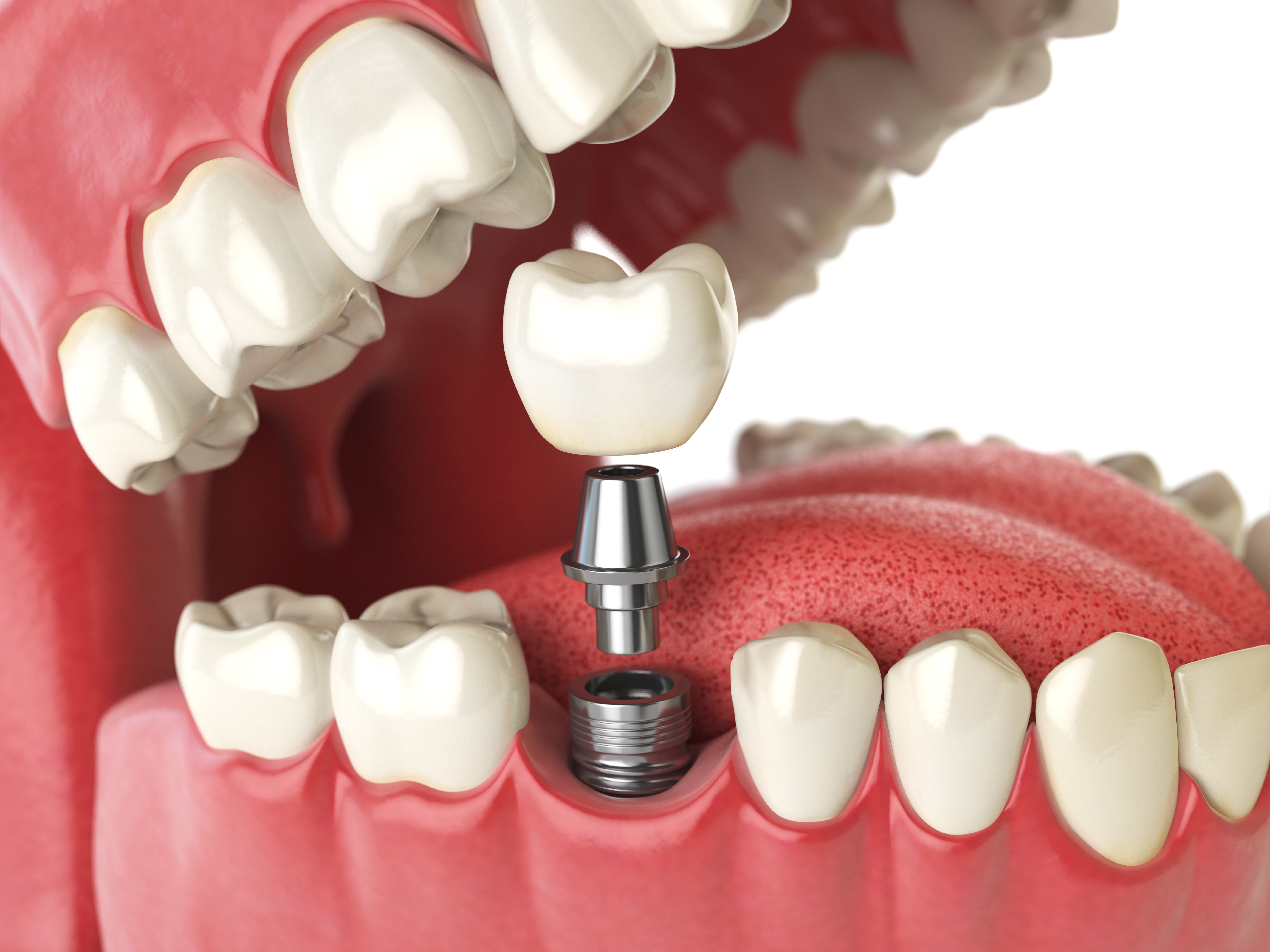
Dental implant restoration combines surgical expertise with advanced material science to replace missing teeth through a systematic approach. The process involves multiple clinical phases where anatomical considerations, diagnostic precision, and material selection work together to establish a stable foundation for tooth replacement.
The Transition from Visible Crowns to Foundational Root Structures
The implant restoration process begins with understanding how artificial root structures integrate with existing bone tissue. Titanium posts serve as the foundational element, designed to mimic natural tooth roots while providing mechanical stability. The crown portion, visible above the gum line, connects to this foundation through an abutment system that transfers chewing forces directly to the jawbone.
The structural design allows for load distribution similar to natural teeth, where forces from chewing and speaking transfer through the crown, down the abutment, and into the titanium post. This mechanical pathway maintains bone stimulation, preventing the deterioration that typically occurs after tooth loss.
The Role of Titanium Osseointegration in Long-Term Stability
Titanium’s biocompatible properties enable direct bone-to-implant contact through osseointegration. This biological process typically occurs over several months, during which bone cells grow directly onto the titanium surface, creating a permanent bond. The integration process depends on factors including bone density, patient health, and surgical technique.
The osseointegration timeline varies based on anatomical location and individual healing capacity. Lower jaw implants often integrate faster due to denser bone structure, while upper jaw placements may require extended healing periods. Surface treatments on titanium implants enhance this integration by creating microscopic textures that encourage bone cell attachment.
Understanding How Surgical Planning Complexity Influences the Overall Procedural Framework
Surgical planning involves comprehensive evaluation of bone structure, soft tissue health, and anatomical limitations. Complex cases requiring additional procedures like bone grafting or sinus lifts extend the overall timeline and increase procedural requirements. Each anatomical variation demands specific surgical approaches and healing protocols.
The planning phase determines the sequence of procedures, healing intervals, and prosthetic design. Simple single-tooth replacements follow straightforward protocols, while full-arch reconstructions require extensive coordination between surgical and restorative phases.
The Anatomical Mapping Required for Precise Placement
Precise implant placement relies on detailed anatomical mapping using three-dimensional imaging technology. CBCT scans provide comprehensive views of bone structure, nerve pathways, and sinus cavities, enabling surgeons to plan exact implant positions while avoiding critical anatomical structures.
Digital planning software allows virtual implant placement before surgery, creating surgical guides that ensure accurate positioning during the actual procedure. This technology reduces surgical time and enhances placement precision, contributing to improved integration outcomes.
Evaluating Initial Clinical Metrics for Structural Support
Bone density measurements determine implant selection and placement strategies. Dense bone provides immediate stability but may require specialized drilling protocols, while softer bone may need longer healing periods or modified implant designs. Bone width and height measurements establish whether additional grafting procedures are necessary.
Clinical evaluation includes assessment of gum tissue health, bite alignment, and adjacent tooth condition. These factors influence the overall treatment approach and prosthetic design considerations.
| Clinical Stage | Procedural Function | Valuation Indicator |
|---|---|---|
| Initial Assessment and Imaging | Comprehensive evaluation and digital mapping | Standard diagnostic protocols and advanced imaging technology |
| Surgical Placement | Implant insertion and primary stability | Titanium grade materials and precision surgical techniques |
| Healing and Integration | Osseointegration monitoring and tissue management | Biocompatible surfaces and guided healing protocols |
| Abutment Connection | Interface establishment and soft tissue shaping | Custom or stock abutment materials and precision manufacturing |
| Final Restoration | Crown fabrication and functional integration | Laboratory-crafted prosthetics and material selection tiers |
Prices, rates, or cost estimates mentioned in this article are based on the latest available information but may change over time. Independent research is advised before making financial decisions.
The Mechanics of Bone Grafting for Structural Reinforcement
Bone grafting procedures address insufficient bone volume through various techniques and materials. Autogenous grafts use the patient’s own bone, while synthetic materials provide alternative options with different integration characteristics. The grafting process requires additional healing time before implant placement can occur.
Graft material selection depends on the defect size and location. Small defects may utilize particulate grafts, while larger reconstructions require block grafts or membrane-guided regeneration techniques. Each approach has specific healing requirements and integration timelines.
How Sinus Lift Procedures Alter the Baseline Timeline
Sinus lift procedures become necessary when upper jaw bone height is insufficient for implant placement. The procedure involves elevating the sinus membrane and placing graft material to increase bone height. This process extends the overall timeline by several months while the grafted area develops adequate bone structure.
Sinus lift techniques vary from lateral window approaches for extensive grafting to less invasive crestal approaches for minor augmentation. The chosen technique depends on the amount of bone augmentation required and the specific anatomical configuration.
The integration of diagnostic technology, surgical precision, and material science creates a comprehensive framework for dental implant restoration. Each clinical phase builds upon the previous stage, establishing the foundation for long-term functional success. Understanding these interconnected elements helps patients comprehend the systematic approach underlying modern implant dentistry and the factors that contribute to successful outcomes.




